Casebook
A Sticky Situation!
As a vet I have seen a huge variety of pet injuries, ailments, misadventures and miraculous recoveries over the years. However, when it was my own dog that experienced a serious medical complaint, it quickly brought home the anxiety that all pet owners must feel when their pet is ill.
Two months ago my one year old Labrador “Luna”, was on her daily walk through the local woodland, this involved running full pelt at every opportunity, sniffing out any tennis ball within a 2 mile radius and consuming as many horse droppings as she can manage. The following day it was noticed that Luna seemed off key, she had vomited once, was reluctant to get out of her bed and there was less ‘wag of the tail’, most alarmingly she didn’t finish her bowl of food that morning. She is normally referred to as the ‘hoover’ due to her legendary Labrador appetite.
I examined Luna and bar a small innocuous scab on her flank, found nothing of concern. I concluded that one mouthful of horse poo too many had been consumed, and treated her for gastro-enteritis. Sadly after a few days it became apparent that Luna was no better and remained subdued and off her food. Further investigation involved blood tests to look at her organ function and blood count, which all came back normal. Further treatment with antibiotics and pain relief provided no improvement and it was elected to progress to imaging. By now I was getting very concerned as Luna had been ill for 7 days.
X-rays taken of Luna’s chest and abdomen showed no abnormalities, however an ultrasound scan of her abdomen showed an irregular mass at the base of her spleen. It was elected to proceed to exploratory surgery which was performed by my colleague Scott Dickson. The result was one of the most surprising of my career. A three inch long section of stick was removed from inside Luna’s abdomen, where it was lodged in lump of scar tissue next to the spleen. There was a considerable amount of infection in the abdomen but fortunately no severe damage to any internal organs.
It appears that the innocuous scab on Luna’s flank was the penetration point of this unusual foreign body, which had proceeded to migrate rapidly through her body wall into the abdomen. This story has a happy ending, and after a long course of antibiotics, Luna has made a full recovery and back to being the ‘hoover’. However, I still watch with bated breath when she runs full pelt through the woodland, though this is part and parcel of Labrador ownership!
Peter Sharp
As a vet I have seen a huge variety of pet injuries, ailments, misadventures and miraculous recoveries over the years. However, when it was my own dog that experienced a serious medical complaint, it quickly brought home the anxiety that all pet owners must feel when their pet is ill.
Two months ago my one year old Labrador “Luna”, was on her daily walk through the local woodland, this involved running full pelt at every opportunity, sniffing out any tennis ball within a 2 mile radius and consuming as many horse droppings as she can manage. The following day it was noticed that Luna seemed off key, she had vomited once, was reluctant to get out of her bed and there was less ‘wag of the tail’, most alarmingly she didn’t finish her bowl of food that morning. She is normally referred to as the ‘hoover’ due to her legendary Labrador appetite.
I examined Luna and bar a small innocuous scab on her flank, found nothing of concern. I concluded that one mouthful of horse poo too many had been consumed, and treated her for gastro-enteritis. Sadly after a few days it became apparent that Luna was no better and remained subdued and off her food. Further investigation involved blood tests to look at her organ function and blood count, which all came back normal. Further treatment with antibiotics and pain relief provided no improvement and it was elected to progress to imaging. By now I was getting very concerned as Luna had been ill for 7 days.
X-rays taken of Luna’s chest and abdomen showed no abnormalities, however an ultrasound scan of her abdomen showed an irregular mass at the base of her spleen. It was elected to proceed to exploratory surgery which was performed by my colleague Scott Dickson. The result was one of the most surprising of my career. A three inch long section of stick was removed from inside Luna’s abdomen, where it was lodged in lump of scar tissue next to the spleen. There was a considerable amount of infection in the abdomen but fortunately no severe damage to any internal organs.
It appears that the innocuous scab on Luna’s flank was the penetration point of this unusual foreign body, which had proceeded to migrate rapidly through her body wall into the abdomen. This story has a happy ending, and after a long course of antibiotics, Luna has made a full recovery and back to being the ‘hoover’. However, I still watch with bated breath when she runs full pelt through the woodland, though this is part and parcel of Labrador ownership!
Peter Sharp

‘THE SHARK MOUTHED DOG’
Harley, a 6 month old female Yorkshire terrier, was brought into our Leith Walk Surgery for routine neutering. However on clinical examination prior to her general anaesthetic, it was found she had two rather than one rows of teeth at the front of her mouth.
Harley’s mouth resembled that of a shark’s mouth with their multiple rows of teeth! So what was this abnormality? Harley had retained deciduous (baby) teeth.
So what’s the problem with a few extra teeth? A retained deciduous (baby) tooth is one that is still present despite the eruption of the permanent tooth (between three to seven months of age). This can cause the permanent teeth to erupt in abnormal positions, resulting in an incorrect bite pattern (how the upper and lower teeth fit together when biting or chewing). Retained deciduous teeth also cause overcrowding of teeth, resulting in food entrapment and subsequent periodontal disease. Therefore retained deciduous teeth should be removed as soon as possible, taking care not to damage the underlying permanent tooth bud. These teeth have normally fallen out by the time of neutering at 6 months and therefore this is the time we normally remove these teeth as the procedure can be carried out under the same anaesthetic.
Harley has 12 retained deciduous teeth removed all together. This was done under general anaesthetic so she was none the wise for her ordeal.
Harley snuggled in a comfy bed after the dental surgery.
Harley, a 6 month old female Yorkshire terrier, was brought into our Leith Walk Surgery for routine neutering. However on clinical examination prior to her general anaesthetic, it was found she had two rather than one rows of teeth at the front of her mouth.
Harley’s mouth resembled that of a shark’s mouth with their multiple rows of teeth! So what was this abnormality? Harley had retained deciduous (baby) teeth.
So what’s the problem with a few extra teeth? A retained deciduous (baby) tooth is one that is still present despite the eruption of the permanent tooth (between three to seven months of age). This can cause the permanent teeth to erupt in abnormal positions, resulting in an incorrect bite pattern (how the upper and lower teeth fit together when biting or chewing). Retained deciduous teeth also cause overcrowding of teeth, resulting in food entrapment and subsequent periodontal disease. Therefore retained deciduous teeth should be removed as soon as possible, taking care not to damage the underlying permanent tooth bud. These teeth have normally fallen out by the time of neutering at 6 months and therefore this is the time we normally remove these teeth as the procedure can be carried out under the same anaesthetic.
Harley has 12 retained deciduous teeth removed all together. This was done under general anaesthetic so she was none the wise for her ordeal.
Harley snuggled in a comfy bed after the dental surgery.
If your pet becomes poorly, or comes home injured, what do you do?
Well if it was us who was feeling unwell, or was lame, we’d reach for the headache relief pills or the anti-inflammatories, right? We would hope to feel better by the next day. So is it OK to do the same and give our cat or dog the same medicines? Then see if they are OK tomorrow?
The answer is a big, straight NO!
By assuming that our pet animals will benefit from the same medicines as people is jumping to a huge and potentially very harmful conclusion. It is true that vets may prescribe the same family of antibiotics that we may receive, or that pets’ diabetes may be treated with a similar insulin but, when it comes to painkillers and anti-inflammatories, there are big differences.
Feeling pretty ropey as a result of a bad cold, or a hangover, we may reach for aspirin as a relief. Surely that would help our poorly cat as well? Well, aspirin CAN be used to treat cats but it lasts much longer in the cat’s body than in ours, making it potentially toxic. High levels of aspirin lead to kidney damage that can be fatal. The only way that aspirin can be used safely in cats is as an anticoagulant in heart and circulatory diseases. In these cases it is used at a very low dose, and is given only once every three days. So, never use aspirin unless your vet prescribes it.
What about Paracetamol then? It is widely and safely used in humans, even in babies – as Calpol – for all sorts of different conditions. If it’s safe for wee kiddies it must be OK for cats and dogs, right? Well, paracetamol is even more dangerous than aspirin, especially in cats. It is a drug with NO veterinary indications, due to its potential toxicity. Cats are very sensitive to paracetamol, where it causes damage to the liver, producing jaundice, anaemia, and blood in the urine. Clinical effects usually occur within 4-12 hours of ingestion. Cats can die of paracetamol poisoning if not promptly treated and, even then, many will not recover. Paracetamol ingestion by a cat is a genuine veterinary emergency.
Among the commonest drugs in the human medicine box is ibuprofen, in its many guises – Brufen, Nurofen, Advil, even types of Anadin. Humans use it by the ton, as part of a cold and flu remedy, for sportsmen and women with sprains and strains, or for sufferers of chronic arthritis and muscular pain, and we can swallow it in liquid or tablet form, or rub it onto local areas as a gel. The dog who comes back limping after hard exercise would benefit from a few days ibuprofen treatment, right? Well actually, no, because ibuprofen kills dogs! It causes toxicity of their kidneys and they can die of kidney failure with vomiting, diarrhoea, anaemia and dehydration.
All of these drugs are members of a group called NSAID’s, or Non-Steroidal Anti-Inflammatory Drugs. Up until about fifteen years ago there was a serious gap in our veterinary pharmacies. When it came to pain relief we had to rely on opiate drugs like codeine, or buprenorphine (Temgesic), or even morphine itself. Then we started to receive new drugs, veterinary NSAIDs, that had the same beneficial effects but without the harmful, toxic side-effects of the human NSAIDs. Even then, some patients would develop less serious side effects, such as tummy upset vomiting and diarrhoea, just as some humans do. In recent years the choice of these drugs has grown, and their effects have become more targeted, and with fewer side effects.
So what’s the best plan when your pet appears poorly or comes home lame? Call your local vet for an appointment, to get him checked out or, if it’s out of hours, ring “e-vets Emergency Service”.
gruff
Gruff is a two year old male Syrian hamster. He presented to our Leith Walk surgery after his owner’s had noticed two very unusual swellings either side of his wind pipe. Gruff was otherwise well but these swellings were growing very rapidly. The decision was made to put him under a general anaesthetic, surgically remove the masses and send them to the pathology lab in order to find out what these masses were.
Such operations are very tricky in hamsters for various reasons, mainly relating to their tiny size. Hamsters are very small animals and therefore a very delicate dissection process is required to remove masses such as these, as they were located very close to some important vessels. Hamsters also lose heat very rapidly, so their body temperature has to be carefully managed whist they are asleep.
Fortunately, Gruff came through his anaesthetic, the operation was a success, and he went home none the wiser. His biopsy results unfortunately were not too good. The pathologist reported a cancer called lymphoma, which is malignant, and which tends to spread to other organs in the body. These tumours can be caused by a virus in young hamsters called hamster polyoma virus, however they can also occur sporadically in older hamsters which is more likely in Gruff’s case.
Gruff is a two year old male Syrian hamster. He presented to our Leith Walk surgery after his owner’s had noticed two very unusual swellings either side of his wind pipe. Gruff was otherwise well but these swellings were growing very rapidly. The decision was made to put him under a general anaesthetic, surgically remove the masses and send them to the pathology lab in order to find out what these masses were.
Such operations are very tricky in hamsters for various reasons, mainly relating to their tiny size. Hamsters are very small animals and therefore a very delicate dissection process is required to remove masses such as these, as they were located very close to some important vessels. Hamsters also lose heat very rapidly, so their body temperature has to be carefully managed whist they are asleep.
Fortunately, Gruff came through his anaesthetic, the operation was a success, and he went home none the wiser. His biopsy results unfortunately were not too good. The pathologist reported a cancer called lymphoma, which is malignant, and which tends to spread to other organs in the body. These tumours can be caused by a virus in young hamsters called hamster polyoma virus, however they can also occur sporadically in older hamsters which is more likely in Gruff’s case.
Max is a lovely, lively and adventurous 7 month old puppy. One afternoon he escaped from the garden when playing with the children. Unfortunately he ran onto the road and got hit by a car, sustaining a sizeable wound to his front left leg.
Max was immediately brought to the vets for treatment – he was given intravenous fluids, painkiller and antibiotics. X-rays were taken and fortunately Max had no internal injuries or major bony damage. The biggest concern was the skin wound on the left front leg.
The wound was initially managed by dressings to accelerate removal of all the contaminated and non-viable tissue. The progress was superb – within days there was evidence of healing with healthy red “granulation” tissue appearing. Max’s owners were great – returning regularly for dressing changes, every time the dressing was spotlessly clean and dry – this must have been quite a challenge considering how lively a puppy Max is.
To aid healing we used an ancient wound covering – HONEY! The Romans used honey to manage wounds though nowadays we get medical grade sterile Manuka Honey to apply to wounds.
Two weeks after the accident Max underwent a general anaesthetic and his wound was reconstructed with a skin graft. The donor skin was taken from his flank and carefully sutured over the wound site. A series of small holes (meshing) were made to allow drainage of fluid from the graft site. Strict immobilization of the graft site is essential for success and the leg was heavily bandaged. Max remained hospitalised during the initial post-operative period to assist healing.
Recovery was fantastic and Max now has a healthy covering of skin over his wound site. In the weeks to come this should be aided by hair regrowth.
Throughout the entire period Max was a model patient, maintaining his usual enthusiasm for life and his owners were great by resting Max throughout the recovery period and keeping his many dressings clean and dry.
Parker was a lively Lionhead rabbit who enjoyed his food and was a faithful house companion for his owner. Parker shared his home with Lou Lou, a recently acquired female rescue rabbit. Rabbits kept together will often become bonded, with mutual grooming and sleeping in contact with each other. However, social interactions between rabbits can be complicated and have some unfortunate outcomes.
Parker was taken to Braid Vets when his owner had noticed an innocuous lump below his left ear. He was well in himself, but the lump was a new development and required investigation. A needle aspirate drew back a thick white material, typical for pus. Infections under the skin in rabbits often result in the formation of thick, tenacious pus. The body reacts to this by ‘walling it off’ to form an abscess with a thick capsule. Abscesses in rabbits are always potentially serious and generally respond best to surgical removal depending on location.
Parker was admitted that day for a general anaesthetic and surgery. The operation proved to be challenging but vet Peter Sharp was able to remove the vast majority of the abscess and capsule. A small section had firmly attached to underlying bone and could not be removed – to deal with this, the surgical wound was partly closed and the cavity was flushed with an antiseptic and antibiotics were given daily.
Fortunately, Parker has made a good recovery and the abscess has healed. It is likely that a bite to the side of his face from Lou Lou was the source of the infection.
Fighting between rabbits is not uncommon and can be significantly reduced if male and female rabbits are neutered. This removes any hormonal drive for aggression. Non hormonal dominant aggression between rabbits can be harder to deal with and will not be resolved by neutering. Introducing a new rabbit ideally involves keeping them in separate cages initially, followed by supervised play in a neutral territory. Over time a bond should develop and hopefully the start of a long and happy friendship!
A Christmas drama for one little dog……
Christmas day is typically enjoyed by all members of the family, including the family pet. Chloe was an affectionate 13 year old West Highland White Terrier, who had enjoyed many years of good health and care from her owners. However, on Christmas day evening, she was rushed in by her owners to E-vets emergency service for a sudden onset of severe vomiting and depression.
Chloe was admitted for treatment with intravenous fluids, antibiotics and pain relief. Despite the initial treatment Chloe’s condition did not improve, she continued to vomit and her breathing became laboured. Further investigation was performed by vet Peter Sharp. X-rays taken showed a severe pneumonia in Chloe’s lungs and a suspicious mass in the mid chest, which may have represented an oesophageal foreign body. After discussion with Chloe’s worried owner, it was decided to perform endoscopy under general anaesthetic. The procedure proved very successful and a large piece of turkey bone ‘knuckle’ was removed with endoscopic forceps from the mid oesophagus.
An oesophageal foreign body is always a severe life threatening emergency. Once the oesophagus is obstructed, the dog is unable to swallow any food, water or saliva and will easily inhale liquid triggering an aspiration pneumonia. The foreign body can also cause severe ulceration of the oesophagus and potentially even cause a rupture.
Chloe needed intensive ‘round the clock’ care, by the veterinary and nursing team for the following 10 days. She was fed through a feeding tube directly into the stomach to bypass the damaged oesophagus, allowing it to heal. Intravenous antibiotics were given to treat the pneumonia and pain relief was provided through out.
Fortunately, Chloe’s story has a happy ending and she has now made a full recovery and is back home with her owners. It appears the turkey bone was consumed in a ‘blink of an eye’ raid on a bin bag on that fateful Christmas day.
Christmas day is typically enjoyed by all members of the family, including the family pet. Chloe was an affectionate 13 year old West Highland White Terrier, who had enjoyed many years of good health and care from her owners. However, on Christmas day evening, she was rushed in by her owners to E-vets emergency service for a sudden onset of severe vomiting and depression.
Chloe was admitted for treatment with intravenous fluids, antibiotics and pain relief. Despite the initial treatment Chloe’s condition did not improve, she continued to vomit and her breathing became laboured. Further investigation was performed by vet Peter Sharp. X-rays taken showed a severe pneumonia in Chloe’s lungs and a suspicious mass in the mid chest, which may have represented an oesophageal foreign body. After discussion with Chloe’s worried owner, it was decided to perform endoscopy under general anaesthetic. The procedure proved very successful and a large piece of turkey bone ‘knuckle’ was removed with endoscopic forceps from the mid oesophagus.
An oesophageal foreign body is always a severe life threatening emergency. Once the oesophagus is obstructed, the dog is unable to swallow any food, water or saliva and will easily inhale liquid triggering an aspiration pneumonia. The foreign body can also cause severe ulceration of the oesophagus and potentially even cause a rupture.
Chloe needed intensive ‘round the clock’ care, by the veterinary and nursing team for the following 10 days. She was fed through a feeding tube directly into the stomach to bypass the damaged oesophagus, allowing it to heal. Intravenous antibiotics were given to treat the pneumonia and pain relief was provided through out.
Fortunately, Chloe’s story has a happy ending and she has now made a full recovery and is back home with her owners. It appears the turkey bone was consumed in a ‘blink of an eye’ raid on a bin bag on that fateful Christmas day.
Name – “Archie”
Age, Sex & Breed – 4 years old, male neutered Cairn Terrier
History – Archie is a bright inquisitive terrier. That afternoon his owner had been about to prepare a chocolate dessert for dinner guests when Archie stole 150g of high quality 70% dark chocolate from the kitchen table.
Examination – Archie had vomited four times by presentation, his heart was going significantly faster than normal and he was dull. Within a short period of time he developed profuse watery diarrhoea. Archie was admitted for hospitalisation and treatment.
Treatment – Archie was given intravenous fluids to aid his circulation and elimination of toxins. He was also given Activated Charcoal by mouth – this is a medication that helps prevent further absorption of toxins. The following day Archie was vastly improved, his vomiting and diarrhoea had ceased and he was discharged with a special highly digestible prescription diet to eat for the next few days.
The Danger of Chocolate Ingestion – Chocolate contains a substance called “theobromine”. The concentration of theobromine varies hugely depending on the type of chocolate – white chocolate has the lowest levels, plain/dark chocolate the highest. In fact plain chocolate can contain over 1500 times the amount of theobromine compared to white chocolate! Chocolate poisoning is a common occurrence – especially at certain times of the year e.g. Easter & Christmas. Archie was fortunate in that his owner sought early veterinary attention. Theobromine can lead to a number of clinical signs, including vomiting, diarrhoea, altered heart speed convulsions and, unfortunately, in some cases it can even be fatal.
Age, Sex & Breed – 4 years old, male neutered Cairn Terrier
History – Archie is a bright inquisitive terrier. That afternoon his owner had been about to prepare a chocolate dessert for dinner guests when Archie stole 150g of high quality 70% dark chocolate from the kitchen table.
Examination – Archie had vomited four times by presentation, his heart was going significantly faster than normal and he was dull. Within a short period of time he developed profuse watery diarrhoea. Archie was admitted for hospitalisation and treatment.
Treatment – Archie was given intravenous fluids to aid his circulation and elimination of toxins. He was also given Activated Charcoal by mouth – this is a medication that helps prevent further absorption of toxins. The following day Archie was vastly improved, his vomiting and diarrhoea had ceased and he was discharged with a special highly digestible prescription diet to eat for the next few days.
The Danger of Chocolate Ingestion – Chocolate contains a substance called “theobromine”. The concentration of theobromine varies hugely depending on the type of chocolate – white chocolate has the lowest levels, plain/dark chocolate the highest. In fact plain chocolate can contain over 1500 times the amount of theobromine compared to white chocolate! Chocolate poisoning is a common occurrence – especially at certain times of the year e.g. Easter & Christmas. Archie was fortunate in that his owner sought early veterinary attention. Theobromine can lead to a number of clinical signs, including vomiting, diarrhoea, altered heart speed convulsions and, unfortunately, in some cases it can even be fatal.
Candy is a spritely 13 year old Golden Retriever.
Presenting Problem – Sudden onset of ‘snorting’ and rasping
History – Candy was a dog that enjoyed a raw carrot as a daily treat from her owner. This healthy snack helped keep her weight trim, teeth clean and had been a longstanding part of the daily routine. However, one evening after finishing her carrot, Candy started with a sudden onset of ‘snorting’ and rasping. By the following morning there was no improvement and Candy was brought in to Braid Vets by her worried owner.
Examination – On examination, vet, Peter Sharp noted that Candy was ‘reverse sneezing’. This is a distinctive noise caused by the ‘aspiration reflex’. This is usually triggered by irritation of the upper surface of the soft palate, which is the fleshy shelf of tissue separating the pharynx (throat) into upper (nasal) and lower (oral) compartments. Reverse sneezing is not uncommon in smaller breeds of dog, especially those with more flattened facial features such as the Pekinese, Lhasa Apso and Chihuahua. Candy was not a typical breed for this behaviour and had never displayed these signs before; consequently a foreign body was considered a possible cause.
Investigation & Treatment – Candy was admitted for a general anaesthetic and exploration of the throat. Endoscopic exam showed that a large piece of carrot was lodged in the nasopharynx above the soft palate. This proved challenging to remove since grab forceps merely ‘pinched’ of small sections of carrot without dislodging it. Eventually the offending foreign body was removed by passing a tube down each nostril into the nasopharynx and flushing the carrot segment into the back of the throat, where it was extracted with forceps.
Outcome – Candy has subsequently made a full recovery from the incident. The cause of the carrot obstruction was sheer bad luck, though it’s fair to say that carrot is now strictly off the menu for Candy!
Presenting Problem – Sudden onset of ‘snorting’ and rasping
History – Candy was a dog that enjoyed a raw carrot as a daily treat from her owner. This healthy snack helped keep her weight trim, teeth clean and had been a longstanding part of the daily routine. However, one evening after finishing her carrot, Candy started with a sudden onset of ‘snorting’ and rasping. By the following morning there was no improvement and Candy was brought in to Braid Vets by her worried owner.
Examination – On examination, vet, Peter Sharp noted that Candy was ‘reverse sneezing’. This is a distinctive noise caused by the ‘aspiration reflex’. This is usually triggered by irritation of the upper surface of the soft palate, which is the fleshy shelf of tissue separating the pharynx (throat) into upper (nasal) and lower (oral) compartments. Reverse sneezing is not uncommon in smaller breeds of dog, especially those with more flattened facial features such as the Pekinese, Lhasa Apso and Chihuahua. Candy was not a typical breed for this behaviour and had never displayed these signs before; consequently a foreign body was considered a possible cause.
Investigation & Treatment – Candy was admitted for a general anaesthetic and exploration of the throat. Endoscopic exam showed that a large piece of carrot was lodged in the nasopharynx above the soft palate. This proved challenging to remove since grab forceps merely ‘pinched’ of small sections of carrot without dislodging it. Eventually the offending foreign body was removed by passing a tube down each nostril into the nasopharynx and flushing the carrot segment into the back of the throat, where it was extracted with forceps.
Outcome – Candy has subsequently made a full recovery from the incident. The cause of the carrot obstruction was sheer bad luck, though it’s fair to say that carrot is now strictly off the menu for Candy!

Toby
Toby is normally a young active cat who enjoys the outdoor lifestyle as much as his home comforts. He was brought to Braid Veterinary Hospital on a Friday morning, after his worried owner noticed he was subdued, off his food and appeared painful over his abdomen.
On examination by vet Peter Sharp it was also noted that his breathing was laboured and his claws were shredded, the latter being a typical sign of trauma, especially road traffic accidents.
Toby was admitted as an emergency for intravenous fluids, pain relief, blood tests and x-rays. The x-rays showed no evidence of serious internal damage to Toby’s organs, though there was some mild anaemia and liver damage on the lab test. Toby responded well to treatment and appeared to make a full recovery with follow up blood tests all within normal limits.
Toby had an uneventful further 2 months until he was seen on a Sunday evening by e-vets emergency clinic, based at Braid Vets Hospital. Again he was subdued and had laboured breathing. Further investigation involved repeat x-rays, which showed a soft tissue mass within the chest cavity, between the lungs and chest wall. An ultrasound exam confirmed this to be Toby’s spleen, which had passed through a tear in the diaphragm (the sheet of muscle separating the abdominal organs from the chest) and was compressing the lungs making it difficult for him to breath.
Toby was rushed to the operating theatre, where surgeon Scott Dickson performed an hour long operation to remove the spleen from Toby’s chest cavity and replace it in the abdomen. The cause of the problem was a tear in the diaphragm .This injury had occurred at the original accident and his spleen had ‘popped ‘through the tear at a later date. It is not unusual for consequences of ruptured diaphragms to be noted several months or even years after the initial trauma.
Toby went on to make a full recovery from the surgery and is back to his normal feisty self, though hopefully being more careful near busy roads!
Toby is normally a young active cat who enjoys the outdoor lifestyle as much as his home comforts. He was brought to Braid Veterinary Hospital on a Friday morning, after his worried owner noticed he was subdued, off his food and appeared painful over his abdomen.
On examination by vet Peter Sharp it was also noted that his breathing was laboured and his claws were shredded, the latter being a typical sign of trauma, especially road traffic accidents.
Toby was admitted as an emergency for intravenous fluids, pain relief, blood tests and x-rays. The x-rays showed no evidence of serious internal damage to Toby’s organs, though there was some mild anaemia and liver damage on the lab test. Toby responded well to treatment and appeared to make a full recovery with follow up blood tests all within normal limits.
Toby had an uneventful further 2 months until he was seen on a Sunday evening by e-vets emergency clinic, based at Braid Vets Hospital. Again he was subdued and had laboured breathing. Further investigation involved repeat x-rays, which showed a soft tissue mass within the chest cavity, between the lungs and chest wall. An ultrasound exam confirmed this to be Toby’s spleen, which had passed through a tear in the diaphragm (the sheet of muscle separating the abdominal organs from the chest) and was compressing the lungs making it difficult for him to breath.
Toby was rushed to the operating theatre, where surgeon Scott Dickson performed an hour long operation to remove the spleen from Toby’s chest cavity and replace it in the abdomen. The cause of the problem was a tear in the diaphragm .This injury had occurred at the original accident and his spleen had ‘popped ‘through the tear at a later date. It is not unusual for consequences of ruptured diaphragms to be noted several months or even years after the initial trauma.
Toby went on to make a full recovery from the surgery and is back to his normal feisty self, though hopefully being more careful near busy roads!
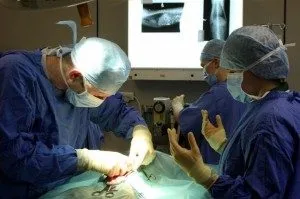
Name – Sylvester
Age & Sex – 13 years old, male neutered.
Breed – Domestic Short Haired Cat
History – Sylvester is a cat who normally enjoys nothing more than a bowl of cat food and the attentions of his owner. He was seen at Braid Vets Leith walk branch on a Monday morning after having been very off colour over the weekend. He was off his food, lethargic and had been sick several times.
Examination – Vet, Christine Ebermeier examined Sylvester and noted he was dehydrated and jaundiced; a yellow discoloration of the eyes, skin and mouth which often indicates a severe liver complaint. Sylvester was admitted to the hospital at 171 Mayfield Road for emergency treatment and intravenous fluids (drip).
Investigation – Peter Sharp had the challenge of investigating Sylvester’s illness. This involved running blood tests using the in-house lab, x-rays and ultrasound examination of the abdomen. These showed that Sylvester had severe liver damage caused by several gallstones that had travelled from the gall bladder, causing an obstruction of the bile duct. If left untreated this would have been a very painful and life threatening condition.
Surgery – Sylvester was rushed to surgery that afternoon where surgeon Scott Dickson carried out a 2 hour operation to remove several gallstones and resect an inflamed infected gall bladder.
Recovery and Outcome – The operation was a great success and Sylvester made a steady recovery over the next few days with the hard work of the veterinary nursing staff.
Biopsy results showed that the cause of the gallstones was an inflammatory condition of the gall bladder and liver, which will require long term management. Sylvester is now eating well and back home with his owner. We are very proud of his recovery from such a serious condition.
Age & Sex – 13 years old, male neutered.
Breed – Domestic Short Haired Cat
History – Sylvester is a cat who normally enjoys nothing more than a bowl of cat food and the attentions of his owner. He was seen at Braid Vets Leith walk branch on a Monday morning after having been very off colour over the weekend. He was off his food, lethargic and had been sick several times.
Examination – Vet, Christine Ebermeier examined Sylvester and noted he was dehydrated and jaundiced; a yellow discoloration of the eyes, skin and mouth which often indicates a severe liver complaint. Sylvester was admitted to the hospital at 171 Mayfield Road for emergency treatment and intravenous fluids (drip).
Investigation – Peter Sharp had the challenge of investigating Sylvester’s illness. This involved running blood tests using the in-house lab, x-rays and ultrasound examination of the abdomen. These showed that Sylvester had severe liver damage caused by several gallstones that had travelled from the gall bladder, causing an obstruction of the bile duct. If left untreated this would have been a very painful and life threatening condition.
Surgery – Sylvester was rushed to surgery that afternoon where surgeon Scott Dickson carried out a 2 hour operation to remove several gallstones and resect an inflamed infected gall bladder.
Recovery and Outcome – The operation was a great success and Sylvester made a steady recovery over the next few days with the hard work of the veterinary nursing staff.
Biopsy results showed that the cause of the gallstones was an inflammatory condition of the gall bladder and liver, which will require long term management. Sylvester is now eating well and back home with his owner. We are very proud of his recovery from such a serious condition.
Name: Tiwi
Each year, usually in Spring or Summer, we see a small number of cases where dogs or cats present with sudden onset sneezing, mild nasal discharge and lots of discomfort. These cases could be the result of an allergic reaction, an acute onset infection, or a nasal foreign body – where something gets stuck up the nostril!
Tiwi, an eight year old Yorkshire Terrier, takes the biscuit though. She has suffered from grass foreign body inhalation twice in one year! On the first occasion, in August 2009, she was brought in showing the typical signs. On closer examination the tip of a grass blade was visible at her nostril and, under a general anaesthetic, two pieces of grass were removed! Tiwi mad a swift and full recovery.
However in June of this year, Tiwi came back again, and with the same symptoms. This time her nostrils looked clear. Again she was anaesthetised and a long blade of grass was removed from the deepest reaches of her nasal cavity. Again she made a complete recovery.
Tiwi loves to root around in long grass and undergrowth and to deny her that would be to deny her one of life’s pleasures. We just hope that next year she doesn’t make it three in a row!
Each year, usually in Spring or Summer, we see a small number of cases where dogs or cats present with sudden onset sneezing, mild nasal discharge and lots of discomfort. These cases could be the result of an allergic reaction, an acute onset infection, or a nasal foreign body – where something gets stuck up the nostril!
Tiwi, an eight year old Yorkshire Terrier, takes the biscuit though. She has suffered from grass foreign body inhalation twice in one year! On the first occasion, in August 2009, she was brought in showing the typical signs. On closer examination the tip of a grass blade was visible at her nostril and, under a general anaesthetic, two pieces of grass were removed! Tiwi mad a swift and full recovery.
However in June of this year, Tiwi came back again, and with the same symptoms. This time her nostrils looked clear. Again she was anaesthetised and a long blade of grass was removed from the deepest reaches of her nasal cavity. Again she made a complete recovery.
Tiwi loves to root around in long grass and undergrowth and to deny her that would be to deny her one of life’s pleasures. We just hope that next year she doesn’t make it three in a row!
Presenting Problem – Vomiting for the past 24 hours and not eating
Name – “Norm”
Age & Sex – 9 months old, male
Breed – Springer Spaniel
Examination – Norm was usually a bouncy happy dog, even when visiting the vets. Today he was looking very sorry for himself – rather than wagging his tail when entering the consulting room Norm chose to lie down, not at all his usual self. No food had been eaten for 2 days. He had a gassy tummy and found it uncomfortable when palpated by the vet, so he was admitted to the hospital for investigation to find out what was the cause of his problem.
Investigation – Norm was put onto Intravenous fluids and given painkillers. Xrays of his abdomen were taken and a blood sample was tested to check out his liver, kidneys and pancreas. His bloods were normal but his xrays revealed abnormally gassy guts – this could be secondary to severe gastro-enteritis or a blockage of his guts. As no foreign body was visible on his xrays Norm was given supportive medication and kept hospitalised for further observation. Overnight he became brighter and did not vomit but his tummy remained uncomfortable.
The next morning his xrays were repeated – his guts were still abnormally gassy. Consent was given by Norm’s owners for exploratory surgery.
Surgery – Under a full general anaesthetic in our sterile operating room, Norm had his abdomen surgically explored. A qualified Veterinary Nurse monitored his anaesthetic whilst the Vet, assisted by another “scrubbed up” Veterinary Nurse, had a thorough examination of his stomach and guts. It did not take long to find the problem – Norm had eaten a sock, which had lodged in Norm’s stomach obstructing the flow of all food.
That however was not all! The elastic of the sock had been chewed loose and had become snagged in a plastic flower that he had also eaten!! This combination of sock elastic and flower had continued to pass through the guts until it could go no further due to the anchoring effect of the sock in the stomach. This had resulted in what is known as a “linear foreign body” with the elastic starting to cut through the gut walls – this was a serious and life threatening problem as if the gut perforated food would leak through and cause peritonitis. No wonder Norm had a sore tummy.
Soon the sock, elastic and plastic flower were removed and Norm was safely stitched up.
Recovery – Norm remained hospitalised for ongoing 24 hour care and observation. Norm received antibiotics, painkillers and more intravenous fluids. Recovery was uneventful and rapid. That evening Norm was looking brighter and even managed a small meal of a special bland diet.
After a further 48 hours Norm returned home, a much happier dog than when he arrived at the vets. He stayed on a special recovery diet for the next 10 days to give his damaged guts a chance to heal, by which point he had fully recovered. Norm made a complete recovery and fortunately has not repeated his dietary indiscretion.
Who would have ever thought that his sore tummy was caused by an unusual snack of a chewed sock and a plastic flower!
Name – “Norm”
Age & Sex – 9 months old, male
Breed – Springer Spaniel
Examination – Norm was usually a bouncy happy dog, even when visiting the vets. Today he was looking very sorry for himself – rather than wagging his tail when entering the consulting room Norm chose to lie down, not at all his usual self. No food had been eaten for 2 days. He had a gassy tummy and found it uncomfortable when palpated by the vet, so he was admitted to the hospital for investigation to find out what was the cause of his problem.
Investigation – Norm was put onto Intravenous fluids and given painkillers. Xrays of his abdomen were taken and a blood sample was tested to check out his liver, kidneys and pancreas. His bloods were normal but his xrays revealed abnormally gassy guts – this could be secondary to severe gastro-enteritis or a blockage of his guts. As no foreign body was visible on his xrays Norm was given supportive medication and kept hospitalised for further observation. Overnight he became brighter and did not vomit but his tummy remained uncomfortable.
The next morning his xrays were repeated – his guts were still abnormally gassy. Consent was given by Norm’s owners for exploratory surgery.
Surgery – Under a full general anaesthetic in our sterile operating room, Norm had his abdomen surgically explored. A qualified Veterinary Nurse monitored his anaesthetic whilst the Vet, assisted by another “scrubbed up” Veterinary Nurse, had a thorough examination of his stomach and guts. It did not take long to find the problem – Norm had eaten a sock, which had lodged in Norm’s stomach obstructing the flow of all food.
That however was not all! The elastic of the sock had been chewed loose and had become snagged in a plastic flower that he had also eaten!! This combination of sock elastic and flower had continued to pass through the guts until it could go no further due to the anchoring effect of the sock in the stomach. This had resulted in what is known as a “linear foreign body” with the elastic starting to cut through the gut walls – this was a serious and life threatening problem as if the gut perforated food would leak through and cause peritonitis. No wonder Norm had a sore tummy.
Soon the sock, elastic and plastic flower were removed and Norm was safely stitched up.
Recovery – Norm remained hospitalised for ongoing 24 hour care and observation. Norm received antibiotics, painkillers and more intravenous fluids. Recovery was uneventful and rapid. That evening Norm was looking brighter and even managed a small meal of a special bland diet.
After a further 48 hours Norm returned home, a much happier dog than when he arrived at the vets. He stayed on a special recovery diet for the next 10 days to give his damaged guts a chance to heal, by which point he had fully recovered. Norm made a complete recovery and fortunately has not repeated his dietary indiscretion.
Who would have ever thought that his sore tummy was caused by an unusual snack of a chewed sock and a plastic flower!
